
Mold Illness: A Practical Guide to Symptoms, Testing, and Recovery
Mold illness—also called mold toxicity or biotoxin illness—happens when people are exposed to mold and the mycotoxins it produces. For many, that exposure leads to persistent, often vague symptoms that interfere with daily life. This guide walks through common signs to watch for, the testing clinicians may use, and practical recovery steps that can help. Early recognition and a focused plan improve outcomes, so we cover symptoms, diagnostics, recovery options, considerations for women and ways to reduce future exposure.
What Are the Common Symptoms and Early Warning Signs of Mold Illness?
Mold-related illness can mimic other conditions, so noticing patterns matters. Early warning signs often include breathing difficulties, persistent fatigue, trouble concentrating, and skin problems. Symptoms may be mild at first and worsen with continued exposure, so spotting changes early lets you pursue appropriate testing and care sooner.
Symptoms frequently follow exposure patterns. Some people feel distinctly better when away from a specific building and worse after returning. Others notice symptoms that track with humidity, recent leaks, or renovation work. Tracking when symptoms appear or improve—and tying them to environments—is a practical step you can take even before formal testing.
Record onset, duration, and triggers. Note indoor spaces where symptoms worsen, any visible water damage, and whether other household members or pets are affected. These observations make clinical conversations more useful and help target environmental assessments.
Which Mold Toxicity Symptoms Indicate Chronic Mold Illness?
When exposure continues over time, symptoms often persist and interfere with everyday functioning. Common long-term signs include:
Respiratory problems: A chronic cough, wheeze, or shortness of breath that doesn’t behave like a routine cold.
Neurological symptoms: Brain fog, memory lapses, trouble concentrating, and mood changes.
Fatigue: Deep, unexplained tiredness or weakness that rest doesn’t fully resolve.
Skin reactions: Rashes, ongoing itching, or other unexplained skin changes.
Because these symptoms overlap with many other conditions, consider the possibility of mold exposure when symptoms don’t respond to usual treatments.
When several systems are affected—for example, respiratory plus cognitive plus skin complaints—clinicians are more likely to investigate an environmental cause. That doesn’t prove mold is responsible, but it raises reasonable suspicion and supports a structured evaluation that includes both clinical and environmental elements.
How Does Mold Exposure Affect Neurological and Immune Systems?
Mycotoxins and related agents can trigger inflammation and disturb immune balance, sometimes producing chronic inflammatory patterns or immune dysregulation. Neurologically, exposure often causes cognitive slowing (brain fog), increased anxiety, or depressive symptoms. Identifying these patterns helps clinicians choose targeted tests and treatments that address both immune and nervous system effects.
Clinicians usually assess symptom clusters, key inflammatory markers, and functional impact when evaluating neurological and immune effects. While bloodwork and specific assays can be informative, the symptom pattern and exposure history guide which tests are most useful. A careful, stepwise approach avoids unnecessary testing and ensures results are interpreted in the context of the whole patient.
Practical self-care while diagnostics proceed includes pacing activities, prioritizing sleep and nutrition, and reducing ongoing exposure. Addressing inflammation and stress early can lessen symptom burden as a comprehensive plan is developed.
How Is Mold Illness Diagnosed Through Testing Methods?
There’s no single definitive test. Diagnosing mold illness typically combines a clinical history, symptom patterns, and targeted laboratory or environmental testing. A thoughtful, combined approach gives the clearest picture and guides effective care.
Diagnosis begins with a careful clinical interview focused on symptom timing, building history, visible or hidden water damage, and any patterns of improvement away from a suspected environment. From there, clinicians select biological tests and environmental assessments that will provide actionable information. A sound diagnostic strategy balances potential benefit, cost, and whether the result will change management.
What Are the Most Accurate Mold Exposure Testing Options?
Common testing approaches include:
Environmental testing: dust-based DNA tests like HERTSMI-2 and ERMI are top recommendations over air or surface swabs, as they better detect historical mold exposure relevant to biotoxin illness.
Serological tests: Blood tests that look for immune responses or antibodies to specific molds.
Urine mycotoxin tests: Tests that measure mycotoxins excreted in urine, which can indicate recent exposure.
Each test has strengths and limitations; often a mix of environmental assessment and biological testing is most informative.
Environmental testing is most useful when it will guide remediation decisions. Finding active mold growth or high airborne spore counts in living areas supports targeted cleanup. But environmental samples must be interpreted alongside a building inspection; isolated positive samples without corroborating evidence are less helpful.
Serological testing can show sensitization to particular molds and may help explain allergic symptoms in the right clinical context. Urine mycotoxin testing can sometimes document recent exposure, but results require clinical correlation and a clear understanding of a test’s validation and limits. Before running tests, discuss with your clinician why each test is being ordered and how the results will influence care.
How Do Urine, Blood, and Nasal Swab Tests Detect Mycotoxins?
Urine mycotoxin tests can reflect recent toxin burden. Blood tests can demonstrate immune activation or antibody responses after exposure. Nasal swabs may detect spores or fungal material in the nasal passages, though they don’t always match systemic illness. Knowing what each test measures helps you and your clinician choose the most appropriate tools.
Timing and preparation matter. For urine testing, some clinicians recommend avoiding certain foods or supplements that might affect results and discussing recent antifungal or antimicrobial use. For blood tests, timing relative to symptom flares or exposures can affect detectability. Nasal swabs are most useful with local nasal symptoms or suspected colonization, but a positive swab alone rarely confirms systemic illness.
Interpretation must account for false positives and negatives. No single result should justify prolonged, aggressive treatment on its own. Instead, look for consistency across history, symptoms, environmental findings, and tests before committing to a long-term plan.
Research clarifies how urine mycotoxin testing is used and how results are interpreted in clinical settings.
Urine Mycotoxin Tests & Mold Illness Diagnosis
A female employee reported new, multi-system symptoms after returning to work following a long absence. Searching online, she found a laboratory offering direct-to-consumer "toxic mold testing" and submitted a urine sample despite no musty odors or visible fungal growth in her office. The laboratory reported positive concentrations for two mycotoxins: ochratoxin at 2.8 parts per billion (ppb) and tricothecenes at 0.4 ppb. The laboratory’s cutoff for a "positive" result was ≥2.0 ppb for ochratoxin and ≥0.2 ppb for tricothecenes. The report’s interpretation stated the results "revealed that you have an unusual level of that mycotoxin(s) present in your body." The laboratory then referred the employee to a clinic that specializes in medical treatment for mold exposure, where she was examined, diagnosed with mold toxicity, and prescribed an antifungal medication.
Notes from the field: use of unvalidated urine mycotoxin tests for the clinical diagnosis of illness—United States, 2014, 2014
Top Home Tests for Mold Illness and CIRS
For individuals with mold illness and Chronic Inflammatory Response Syndrome (CIRS), dust-based DNA tests like HERTSMI-2 and ERMI are top recommendations over air or surface swabs, as they better detect historical mold exposure relevant to biotoxin illness.
HERTSMI-2
HERTSMI-2 screens dust for 5 key toxigenic molds linked to CIRS. Scores under 11 are considered safe, 11-15 borderline, and over 15 unsafe. This test costs between $130 and $265 and is available via EnviroBiomics Swiffer kits. It is ideal as an initial screening tool.
ERMI
ERMI analyzes dust for 36 mold species, providing a relative moldiness score. For CIRS sensitivity, a score under 2 is desirable. ERMI is more comprehensive but also pricier, ranging from $240 to $435.
EnviroBiomics Panel #7 (SM-AEH)
This panel combines HERTSMI-2, Actinomycetes (actinos), and Endotoxins, making it essential for a full biotoxin assessment in CIRS-affected homes. Samples are collected using Swiffer cloths after 2-6 weeks of dust buildup.
Why These Tests Excel for CIRS
These MSQPCR dust tests from labs like EnviroBiomics capture settled spores and biotoxins that air sampling often misses. The CDC and CIRS experts consider air sampling unreliable for chronic illness. EMMA testing adds mycotoxins but costs more and overlaps with Panel #7.
Safe Score Thresholds
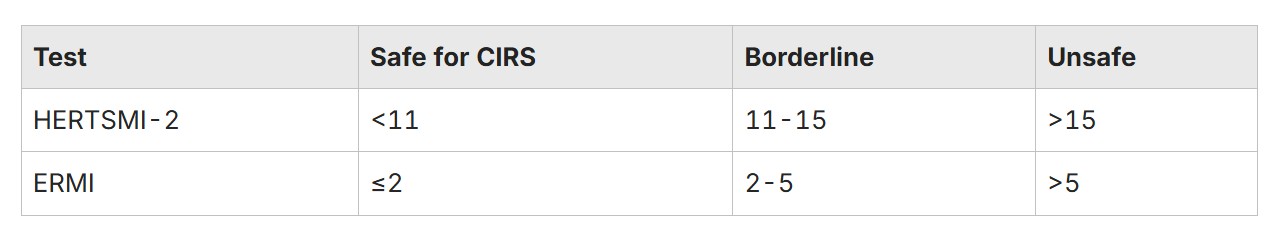
Collect samples from multiple rooms such as vents and floors, and avoid testing immediately after cleaning. Retesting 2-6 weeks after remediation is recommended. Consult a CIRS-aware practitioner to interpret results and guide next steps.
What Are Effective Recovery Protocols and Mycotoxin Detox Strategies?
Recovery from mold-related illness usually requires several coordinated steps: stop ongoing exposure, support the body’s detox pathways, address inflammation, and rebuild overall resilience with lifestyle and medical supports. A personalized plan typically yields the best results.
Start with exposure control. If your home or workplace is the likely source, remediation or temporary relocation should come first. At the same time, work with a clinician to manage symptoms and guide testing so you avoid unnecessary or potentially harmful interventions. Recovery is often gradual and benefits from clear priorities and realistic milestones.
Key clinical supports commonly include symptom-directed therapies (for breathing, sleep, mood, and pain), anti-inflammatory strategies, and stepwise efforts to improve metabolic and detoxification capacity. Mental health care is important too—chronic symptoms are stressful, and addressing anxiety, sleep disruption, and coping skills speeds recovery.
Which Detoxification Protocols Support Chronic Mold Illness Treatment?

Common elements in detox and recovery plans include:
Dietary changes: A mainly anti-inflammatory, nutrient-dense diet rich in antioxidants to support healing and toxin clearance.
Supplementation: Targeted supplements—such as certain binders and antioxidants like glutathione—may help lower toxin burden when used under medical supervision.
Sauna therapy: Regular, supervised sauna use can promote sweating and support elimination pathways for some patients.
Clinical and experimental work shows that adsorbent materials like activated carbon and cholestyramine can reduce intestinal uptake of certain mycotoxins.
Activated Carbon & Cholestyramine for Mycotoxin Detoxification
The addition of activated carbon or cholestyramine to diets contaminated with mycotoxins significantly reduced intestinal absorption of those mycotoxins compared with untreated diets.
Recent advances on the use of adsorbent materials for detoxification of Fusarium mycotoxins, G Avantaggiato, 2005
Used alongside exposure control and supportive care, these strategies can strengthen natural detox pathways and aid recovery.
Because supplements and detox therapies can interact with medications and underlying conditions, use them only under clinical supervision. Start at low doses, monitor symptoms, and reassess labs or clinical endpoints as your provider recommends. Track changes so you can identify which parts of a protocol are helping.
Practical recovery checklists often emphasize prioritizing sleep, stabilizing blood sugar with balanced meals, gentle daily movement as tolerated, slowly returning to work or social activities, and scheduled follow-ups with clinicians during recovery.
How Long Is the Typical Mold Illness Recovery Timeline?
Recovery timelines vary widely. Some people feel better within weeks after exposure is stopped and supportive care begins; others require several months for meaningful improvement. Speed of recovery depends on exposure duration and intensity, how quickly sources are removed, adherence to treatment, and underlying health issues.
Clinicians often use a staged timeline to set expectations: early stabilization (weeks) focuses on symptom control and exposure removal; mid-phase recovery (months) emphasizes rebuilding resilience and function; long-term maintenance (months to a year or more) centers on preventing relapse and sustaining gains. Regular reassessment helps adjust care and avoids stopping useful therapies too soon.
Seek prompt reassessment for red flags such as worsening respiratory compromise, rapidly progressive neurological signs, or new objective findings that suggest a different diagnosis. If these occur, return to medical care right away.
What Special Considerations Exist for Women Aged 35-60 with Mold Illness?
Women roughly 35–60 years old may face extra challenges because hormonal changes during this period can magnify symptoms. A personalized plan that accounts for hormonal and metabolic health often improves outcomes.
Hormonal shifts—whether perimenopausal, menopausal, or related to other reproductive issues—can affect sleep, mood, and energy, which in turn influence tolerance for environmental stressors. Addressing hormonal health can therefore be a useful part of a multi-pronged recovery plan.
How Does Mold Illness Manifest Differently in Women 35-60?
Clinical experience suggests women in this age group may report more pronounced neurological symptoms, including anxiety and depression. Hormonal fluctuations can alter symptom severity and recovery, so treatment plans should consider gender-specific factors.
Because women in this range often face overlapping issues—sleep disturbance, metabolic shifts, and life stressors—coordinating care between environmental medicine, primary care, and women’s health specialists creates a more cohesive plan. Simple steps like checking vitamin D and iron, and improving sleep hygiene, can make other therapies more effective.
Which Personalized Programs Address Chronic Environmental Illness in This Group?
Programs tailored for women in this age range commonly include:
Hormonal balancing: Evaluating and addressing hormonal imbalances that may worsen symptoms.
Nutritional support: Customized dietary plans to support detoxification, hormone balance, and energy.
Mind-body therapies: Stress-reduction practices such as yoga, meditation, and breathwork to strengthen resilience and mental health.
These personalized strategies can help women manage symptoms more effectively and support long-term recovery.
Additional supports may include bone and cardiovascular risk assessments when appropriate, targeted physical therapy to rebuild stamina, and counseling to address work-life adjustments during recovery. Integrating practical interventions with medical care reduces trial-and-error and speeds functional improvement.
How Can Prevention and Environmental Controls Reduce Mold Exposure Risks?
Prevention is the most effective long-term strategy. Practical environmental controls and routine maintenance dramatically lower the risk of future illness.
Focus on moisture control. Small leaks or elevated indoor humidity create conditions where mold thrives. Early detection and repair are less costly and more effective than large-scale remediation after growth is established.
What Environmental Measures Minimize Mold Growth and Mycotoxin Exposure?
Key preventive steps include:
Humidity control: Keep indoor humidity below 50% to discourage mold growth.
Proper ventilation: Ensure good airflow in bathrooms, kitchens, and other damp areas to limit moisture buildup.
Regular inspections: Check for leaks, water damage, and hidden damp spots so problems are fixed early.
These consistent habits make indoor spaces healthier and reduce the chance of mold-related health problems.
Practical tips include using exhaust fans while showering or cooking, placing dehumidifiers in basements or crawlspaces prone to dampness, and avoiding carpeting in frequently wet areas. When cleaning small, visible mold patches, use appropriate PPE (gloves, mask) and non-ammonia cleaners; for larger or hidden contamination, hire a qualified remediation professional who follows containment and cleanup standards.
If you suspect a building issue, document visible damage and odors, take dated photos, and keep repair and remediation records. These notes help clinicians and remediation specialists assess risk and plan effective interventions.
How Does Early Detection Prevent Chronic Inflammatory Response Syndrome?
Early identification of mold exposure and appropriate testing can reduce the risk of developing chronic inflammatory response syndrome (CIRS), a complex condition linked to prolonged exposure. Recognizing symptoms early and acting quickly—both clinically and environmentally—improves the chance of avoiding long-term complications.
Early steps include prioritizing exposure control, addressing inflammation, and monitoring for improvement. If symptoms persist despite reasonable interventions, a structured specialist evaluation can refine diagnosis and treatment. Time matters: the sooner exposure is controlled, the greater the likelihood of a fuller recovery.
Careful diagnosis of CIRS is important because confirmation often requires both clinical improvement and sufficient time for recovery.
Diagnosing Chronic Inflammatory Response Syndrome (CIRS)
Chronic inflammatory response syndrome (CIRS) was first described in 1997 (Shoemaker 1997). This work is among the earliest to report prevalence and compare different diagnostic approaches against the two case definitions (CD) in the literature. Both CDs require clinical improvement with therapy to confirm the diagnosis (Shoemaker and House 2006, GAO 2008). Compliance can be difficult, and improvement may take months; definitive diagnosis using the CDs therefore requires time. In a review of 1,061 consecutive patients of all ages seen at a CIRS specialty clinic, 371 met CIRS criteria.
An evaluation of alternate means to diagnose chronic inflammatory response syndrome and determine prevalence, 2017
How Does Genetic Susceptibility Influence Mold Illness?
Genetic factors can play a significant role in how individuals respond to mold exposure. One key genetic component is the HLA-DR gene, which is part of the human leukocyte antigen system involved in immune regulation. Variations in this gene affect the body's ability to recognize and clear biotoxins produced by mold and other environmental sources.
People with certain HLA-DR gene variants may have a reduced capacity to effectively eliminate these biotoxins, making them more susceptible to developing chronic symptoms after mold exposure. This genetic susceptibility helps explain why some individuals, particularly women, struggle more with mold illness and Chronic Inflammatory Response Syndrome (CIRS) despite similar environmental conditions.
Understanding your HLA-DR status can provide valuable insight into your risk and guide personalized treatment strategies. For a deeper exploration of this topic, including why some women face greater challenges clearing biotoxins, see our detailed article: Understanding the HLA-DR Gene: Why Some Women Struggle to Clear Biotoxins.
What Are Frequently Asked Questions About Mold Illness Symptoms, Testing, and Recovery?
People commonly ask the same core questions about symptoms, which tests to trust, and what recovery looks like. Clear answers help you make informed choices and work with clinicians more effectively.
Can Mold Illness Be Cured and What Are the Treatment Success Rates?
A complete “cure” isn’t guaranteed for everyone, but many people achieve substantial symptom relief and improved daily function with a comprehensive plan that removes exposure, treats inflammation, and supports detoxification. Success depends on factors such as how early exposure is identified and how thoroughly it’s addressed.
Successful recovery usually reflects a combination of removing or minimizing exposure, guided medical care, and sensible lifestyle changes. Patients who engage in coordinated care, follow environmental advice, and address sleep, nutrition, and stress typically report better outcomes. Regular follow-up and readiness to adjust treatment based on progress are important.
Which Tests Are Recommended for Accurate Mold Toxicity Diagnosis?
A mix of environmental testing, urine mycotoxin testing, and targeted serological tests is often recommended to build a complete clinical picture. Working with a clinician who understands both environmental assessment and biological testing gives the best chance of an accurate diagnosis.
Other common questions include:
When should I see a specialist? Consider referral if symptoms persist despite removing obvious exposure, if multiple body systems are affected, or if standard treatments aren’t helping. Environmental health or occupational medicine specialists can be helpful.
Are home test kits reliable? Home kits vary widely in quality and interpretation. Use results as one part of an overall assessment and discuss findings with a clinician or qualified environmental professional before making major medical or remediation decisions.
Can pets be affected? Yes—pets can show respiratory or skin issues in damp, moldy environments. Veterinary evaluation and an environmental assessment are useful if multiple household members, including animals, are symptomatic.
What about insurance and costs? Coverage varies by plan and region. Discuss likely costs, which tests are medically necessary, and whether remediation will be covered or require out-of-pocket payment.
Finally, build a simple plan: document symptoms and exposures, prioritize source control, work with a clinician to choose targeted testing, and use staged recovery steps to rebuild function. This practical approach reduces uncertainty and supports steady progress toward better health.
Need Support with Mold Illness? Contact Janice Maynard, FDN-P
If you suspect you have mold illness or are struggling with symptoms related to mold exposure or Chronic Inflammatory Response Syndrome (CIRS), consider reaching out to Janice Maynard, FDN-P, at Rejuvenate Your Life Holistic Wellness. Janice is a toxic mold trained practitioner who has personally experienced mold illness and CIRS, bringing both professional expertise and lived experience to her care approach.
Janice offers personalized guidance, testing support, and recovery protocols for all natural self treatment tailored to your unique needs. To book a consultation, visit her booking page. You can read more about Janice and Rejuvenate Your Life Holistic Wellness here.
Additionally, you can download a free, informative PDF titled "The Truth About Mold Illness: What Doctors Don't Tell You" to learn more about mold illness, common misconceptions, and practical steps for recovery.
Taking early action and working with a knowledgeable practitioner can make a significant difference in your recovery journey. Don’t hesitate to seek support and empower yourself with trusted information and care.
